Authors
Recent federal proposals have renewed focus on price transparency as a tool for lowering healthcare costs. These initiatives rely on a fundamental assumption that increased transparency will drive competition and bring prices down. But does that assumption actually hold? To answer that question, we looked at prices in one of the most expensive, complex, and financially toxic areas of healthcare: cancer care.
In a new study we co-authored with researchers at Memorial Sloan Kettering Cancer Center, we examined whether price transparency is associated with changes in oncology prices, and under what conditions. To our knowledge, this study provides the first evidence linking the effectiveness of hospital price transparency to both the extent and the completeness of price disclosures. Let’s walk through our key findings.
More Transparency, Bigger Price Cuts
We analyzed insurer-negotiated prices for 89 oncology services at 228 hospitals across the 10 largest U.S. metropolitan areas between December 2021 and June 2024. The big takeaway: services with more extensive price disclosures showed larger subsequent price cuts.
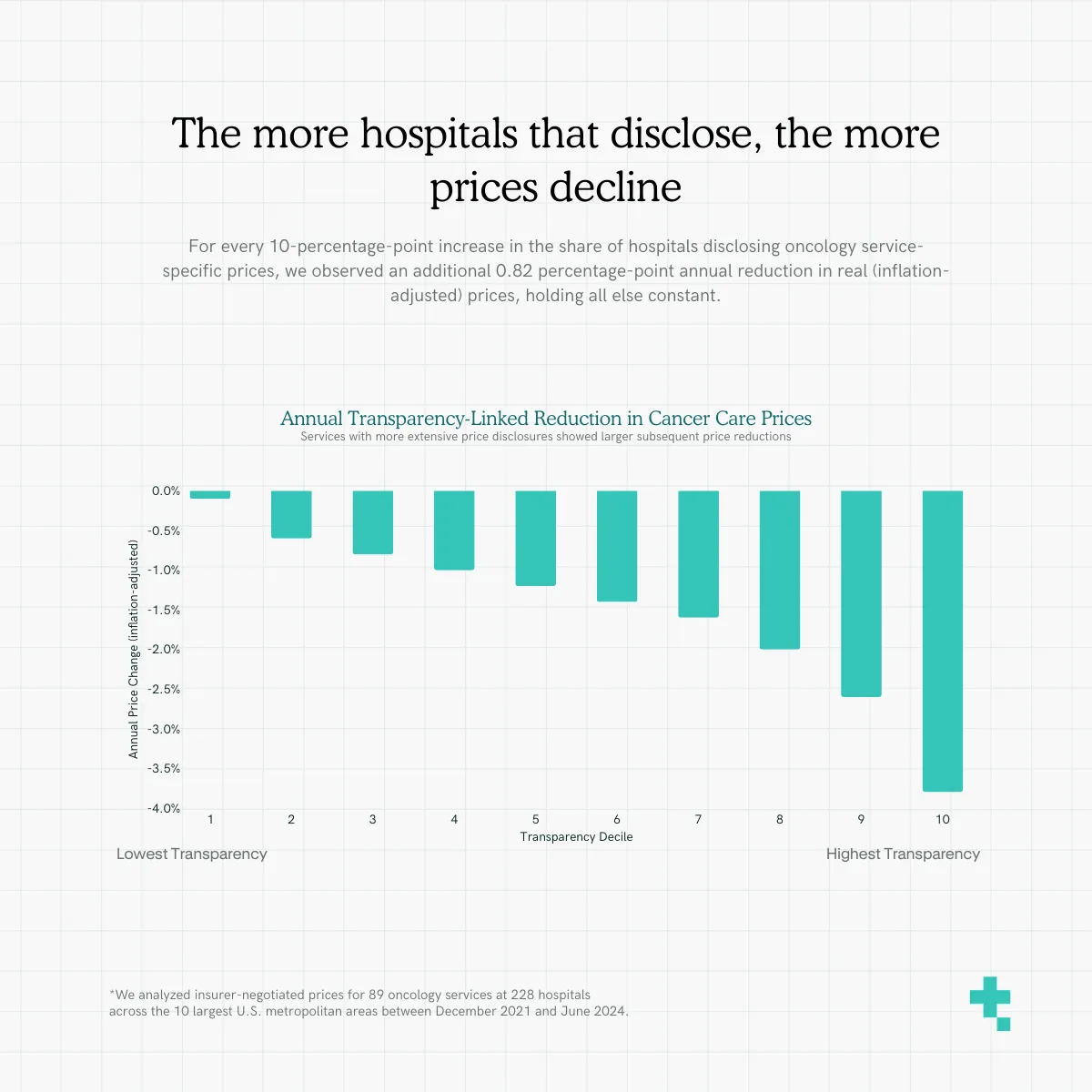
The more hospitals that disclose, the more prices decline
For every 10-percentage-point increase in the share of hospitals disclosing oncology service-specific prices, we observed an additional 0.82 percentage-point annual reduction in real (inflation-adjusted) prices, holding all else constant. This is consistent with economic theory. When more hospitals disclose prices for a service, it enables meaningful price comparisons and competition, putting downward pressure on prices for that service.
Simply posting files is not linked to lower cancer care prices
What doesn’t appear to work? Simply posting a machine-readable file (MRF) without disclosing prices for specific oncology services. Although hospitals are required to disclose prices for “all items and services,” we observed a median of only 19.0% of hospitals in each metro disclosing oncology service-specific prices at the start of the study period. A much higher proportion of hospitals (median of 47.9%) had posted machine-readable files. A natural question is whether partial price disclosures are enough to stimulate broader price competition and reduce prices across services. We found no evidence of that. MRF posting alone was not associated with changes in oncology prices.
Together, these findings suggest that price transparency is not binary. Transparency exists on a spectrum, and only disclosures that enable service-specific price comparisons appear to reduce prices.
Not All Services (or Hospitals) Are Created Equal
Price transparency is not the only force shaping oncology price dynamics. Real price trends varied significantly across service categories and hospital characteristics, independent of disclosure levels.
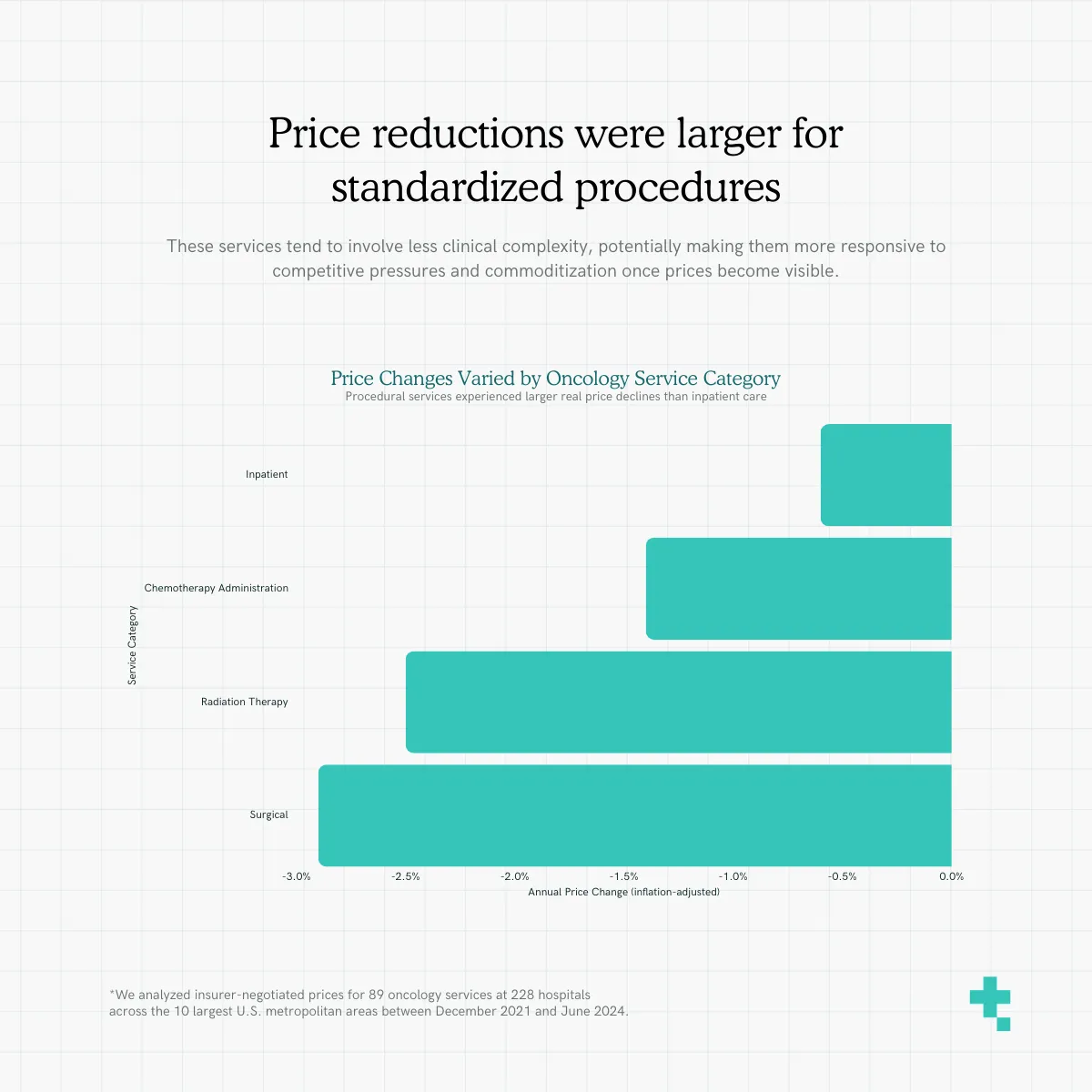
Price reductions were larger for standardized procedures
Price reductions were larger for more standardized, procedural services such as radiation therapy and surgical procedures than for inpatient cancer care. These services tend to involve less clinical complexity, potentially making them more responsive to competitive pressures and commoditization once prices become visible.
Not all factors were associated with price declines
Larger hospitals experienced greater price increases over time, with each additional 100 beds associated with a 0.6 percentage-point increase in oncology prices each year. Larger hospitals tend to have greater market power, as well as more sophisticated contracting and analytics capabilities that may allow them to better leverage pricing data in contract negotiations.
The Convergence Effect
Beyond changes in average prices, we also examined how the variation in prices changed within markets. Consistent with prior analyses, we observed price convergence. Over time, prices for the same cancer service became more uniform within each metro.
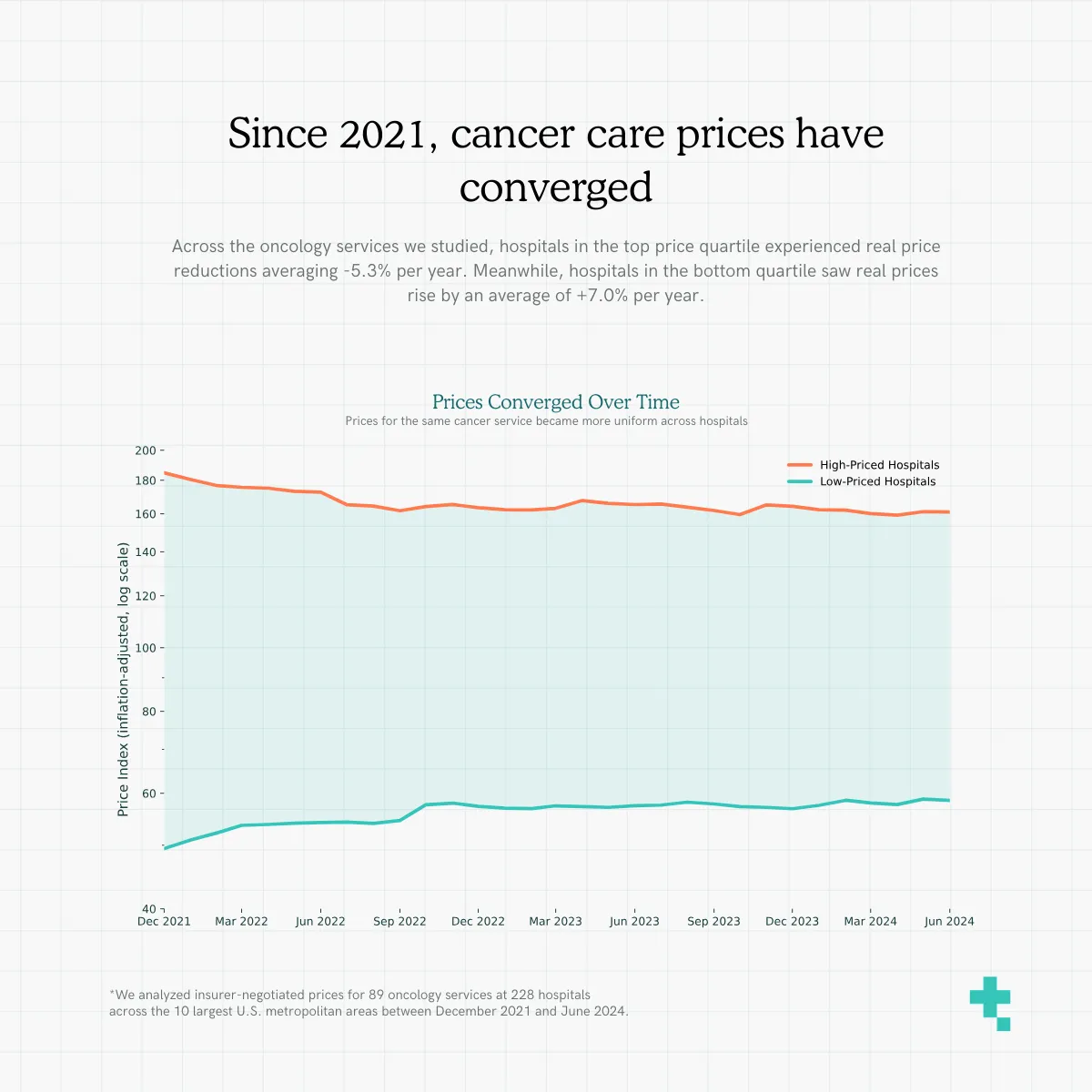
The gap between high-priced and low-priced hospitals narrowed
Across the oncology services we studied, hospitals in the top price quartile experienced real price reductions averaging -5.3% per year. Meanwhile, hospitals in the bottom quartile saw real prices rise by an average of +7.0% per year. After controlling for service category, payer, and market structure, the gap between the highest- and lowest-priced hospitals narrowed at an average rate of 21.2 percentage points per year.
Price convergence wasn't associated with the extent of price disclosures
Interestingly, we found that price convergence was not associated with the extent of price disclosures. Why would this be the case? One plausible explanation is anchoring. You don't need every hospital to publish prices to set a benchmark. Once a price anchor is established, it constrains outlier prices, pulling high-priced hospitals down while giving low-priced hospitals the leverage to negotiate up. In contrast to the price reductions described above, which were associated with extensive, service-specific disclosures, price convergence can occur even following baseline levels of price disclosure.
A Tale of Two Dynamics
The findings above highlight two distinct pricing dynamics:

These dynamics have different policy implications. Downward repricing provides a mechanism for lowering healthcare costs. Price convergence, however, is more ambiguous. While it reduces prices at the high end, it can also limit access to the lowest-priced care options as prices rise at historically inexpensive hospitals.
Please note
It’s important to note that these pricing dynamics reflect insurer-negotiated prices for oncology services in large metropolitan markets and may not generalize to other services or regions. In addition, because comprehensive pre-transparency pricing data are not available, the analysis is observational and identifies associations rather than causal effects. Whether these dynamics translate into more affordable care depends on how stakeholders across the healthcare sector respond.
So How Do We Make Cancer Care More Affordable?
Our research suggests that price transparency can play a meaningful role in reducing prices in cancer care. While these early findings are promising, as transparency moves from policy to practice, the real-world impact of transparency will depend on how healthcare stakeholders respond. Our findings have important implications for three groups in particular:
For Policymakers
Complete and extensive disclosures are critical for reducing prices. The simple act of publishing an MRF was not associated with price reductions. Instead, price reductions were associated with widespread publication of service-specific price disclosures. Broad price reductions are less likely without strict enforcement of price transparency rules, which helps ensure that all hospitals publish complete MRFs with prices for all items and services.
Price transparency can also have unintended side effects. While greater enforcement may increasingly drive average prices down, as the spread of prices for each service narrows, prices at historically low-priced hospitals are rising. Policymakers may need to monitor these options to ensure continued access to affordable care.
For Hospitals
Pricing data has become table stakes in negotiations. Payers and providers are coming to the table with an increasingly consistent set of benchmark prices. Against this backdrop, we are seeing prices for each service becoming more uniform as they converge towards a standard market rate.
However, transparency has not eliminated differences in market power. Larger hospitals are showing price increases relative to smaller peers, highlighting that pricing data may be used by these well-resourced, analytically sophisticated systems to maintain pricing leverage. These negotiation outcomes will shape the broader affordability of cancer care.
For Patients
Prices are still mostly invisible outside of MRFs. Today, prices are moving behind the scenes in payer-provider contract negotiations. While lower negotiated rates are an important first step, they do not automatically translate to lower out-of-pocket costs. Future work will be needed to quantify the downstream impact on patients. And, perhaps just as crucially for patients, using data from MRFs to create more accurate patient estimate tools can help give patients and their care teams more clarity around cost.
Price transparency continues to hold merit
Ultimately, our research suggests that price transparency can be a valuable method of improving healthcare affordability, but the implementation must enable service-specific price competition. More extensive, complete disclosures are associated with larger price reductions, while partial transparency has limited effects.
Strict enforcement of complete MRFs has the potential to drive additional price reductions. As transparency policies mature, the line between meaningful disclosure and box-checking may determine whether transparency becomes a true cost-control tool or just another reporting requirement.
See inside the black box
Traceable data, unified workflows, and total transparency
Related resources
Learn, listen, and watch the latest on price transparency.

Introducing the Turquoise Out-of-Network Dashboard
Turquoise launched a free, open license out-of-network pricer built on data designed to eliminate the opacity in QPA calculations, IDR disputes, and broader OON pricing scenarios.


