Authors
Thanks to the hard work of many managed care teams across the US, baseline price transparency compliance is now nearly universal. At the time of writing, 91% of payer files pass the technical bar for CMS schema compliance and 44% of hospitals are fully compliant with CMS machine-readable file requirements, with over 91% of hospitals having adopted the most up-to-date file requirements. Despite some policy clunkiness, Executive Orders, final rules, and schema updates have solidified transparency’s first chapter. It’s incredible! The industry has changed before our eyes. And the people want to know: what’s next?
For five years, reform has meant rules, schemas, and compliance deadlines. While that was necessary, the progress made opens the floor for deeper reform work to begin in how the industry writes, negotiates, and understands its contracts: the very language that determines the price of healthcare in the U.S..
While we wait and see what 2026 policy might bring, your friends here at Turquoise believe the next phase of reform in healthcare won’t just come from Washington. We think it’ll come from within the industry itself, from the leaders ready to turn transparency into efficiency and contracts into catalysts for reform.
Policy has cleared the way for workflow evolution
While healthcare is intimately familiar with technological innovation on the clinical side, the backoffice hasn’t had the same privilege. Due to the vast, nuanced, and often perplexingly complicated nature of our healthcare administration system, creating tech-forward solutions that don’t further bloat the system or exacerbate the backoffice’s siloed-tech problem has been a challenge. As a result, the backoffice is stuck levering tech from the 80’s and present day simultaneously. Every organization harnesses a different cocktail of new and old technologies to conduct negotiations and day to day business—none of them, none, talk to each other and all of them were created to solve one niche microcosm. The result is a woefully disjointed, staccato backoffice stuck making do. With countless medical claims working their way through the revenue cycle each year, this hodge-podge techstack isn’t serving anyone anymore.
The US wastes $570B a year on inefficient admin. CFOs are facing more pressure than ever to tighten processes and invest in AI. As our CEO, Chris Severn, said in a recent webinar about AI and contacting, “AI is everywhere in the news… but how is it actually relevant to your roles in payer-provider contracting? It isn’t about generative text, servers, or models. It’s about the actual workflows that matter.” Turquoise’s product ethos has always been about bringing the best of technology from other industries into healthcare. Now that transparency has been integrated into the everyday processes of the backoffice, a new quiet revolution is happening: a shift from compliance to capability.
Deeper backoffice reform doesn't have to wait for Washington. It can start in how we negotiate, analyze, and standardize value itself.
Contracts: Healthcare’s model candidate for reform
Literally every dollar of healthcare runs through a contract. But those contracts are unstructured, unstandardized, and worst of all: meaningfully inaccessible to the very CFOs held accountable to them.
As Chris explained in the webinar, AI can now detect underpayments and predict negotiation outcomes or gaps, but only if the underlying contracts speak a common, standardized, language. With our intelligent contracting platform, Clear Contracts, AI reads, compares, and reconciles those micro-policies faster than any human. It surfaces predictive insights and exposes underpayments or inefficiencies. Those aren’t headache-inducing compliance exercises or generative text kindly writing your emails. They’re practical, achievable reform in motion.
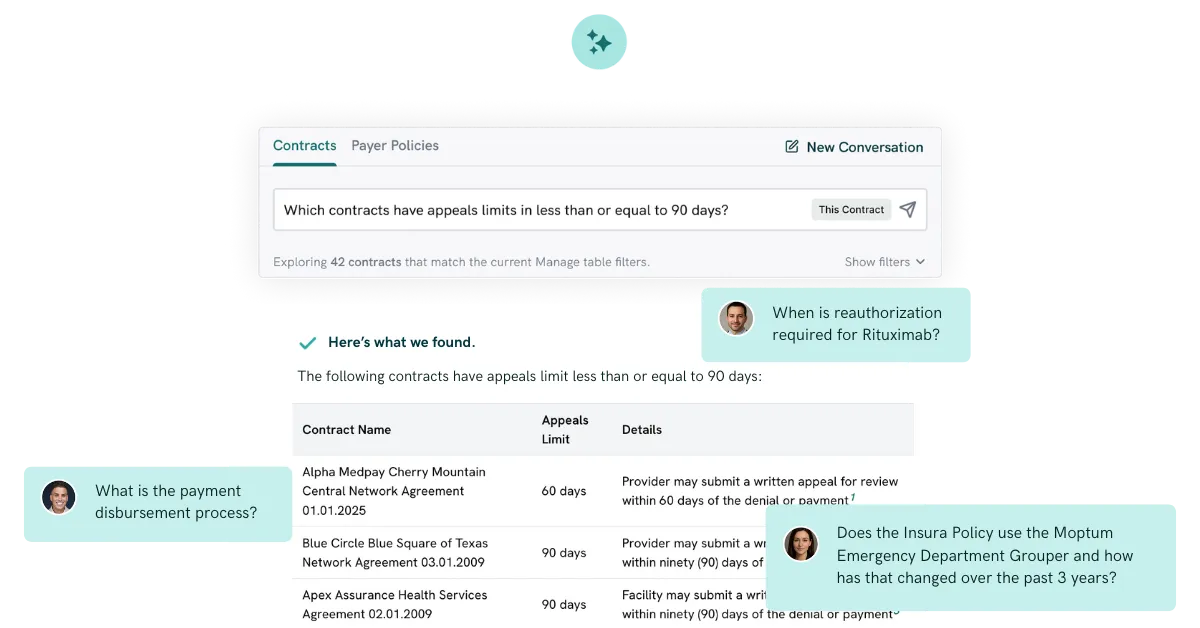
Standardization isn't just good governance, it's technical hygiene. This has been a major challenge to overcome in our own product building. To do this, we’ve undergone exhaustive trial and error to develop a standard method of contract organization. On the policy side, we’re rallying around a PADU (Preferred, Acceptable, Discouraged, and Unacceptable) framework: an industry-led library of preferred and discouraged contract terms that replaces opacity with mutual accountability.
Other sectors have already proven healthcare can standardize the seemingly un-standardizable to great effect:
- Finance: The ISDA Master Agreement made global trading possible
- Tech: SLAs defined reliability and performance for cloud computing
- Real Estate: Fannie Mae and Freddie Mac brought standardization and security to the US mortgage market
Each of these industries reached their own tipping points where bespoke agreements stopped meaning “competitive" and instead became woefully wasteful. If healthcare were looking at a map, the “YOU ARE HERE” sticker is right here. The next evolution of transparency isn’t continued iterations of disclosure, its translation. Accuracy and completeness still matter, but clarity is what makes them usable
The next frontier of transparency won’t come from new rules alone. It will come from the shared architecture of contracts built collaboratively by payers, providers, and innovators. Contracts should be easily accessible and understood by humans, auditable by machines, and comparable across organizations. When that happens, every CFO, revenue cycle leader, and contract analyst will finally operate from the same source of truth.
Policy may have cleared the way (dear CMS: hey, thanks!) but the future belongs to the industry innovators within healthcare (reader, we mean you) who have the power and responsibility of turning fine print into board-approved frameworks that deliver year over year. Reform won’t just come from another rule, it’ll come from common language that makes healthcare’s fine print understandable, trustworthy, and ultimately, functional.
The right tech for the job
So how do we do it?! While AI is in every AI-generated headline, it’s not the hero of this story—people are (aww!). Tech won’t drive reform here, people will. AI will enable people to make that reform stick.
AI is the translator, not the negotiator or CFO. It can, and arguably is best at, turning data into a daily decision-making tool. That’s the kind of reform that lasts. Not because it’s mandated (though, love) but because it’s useful.
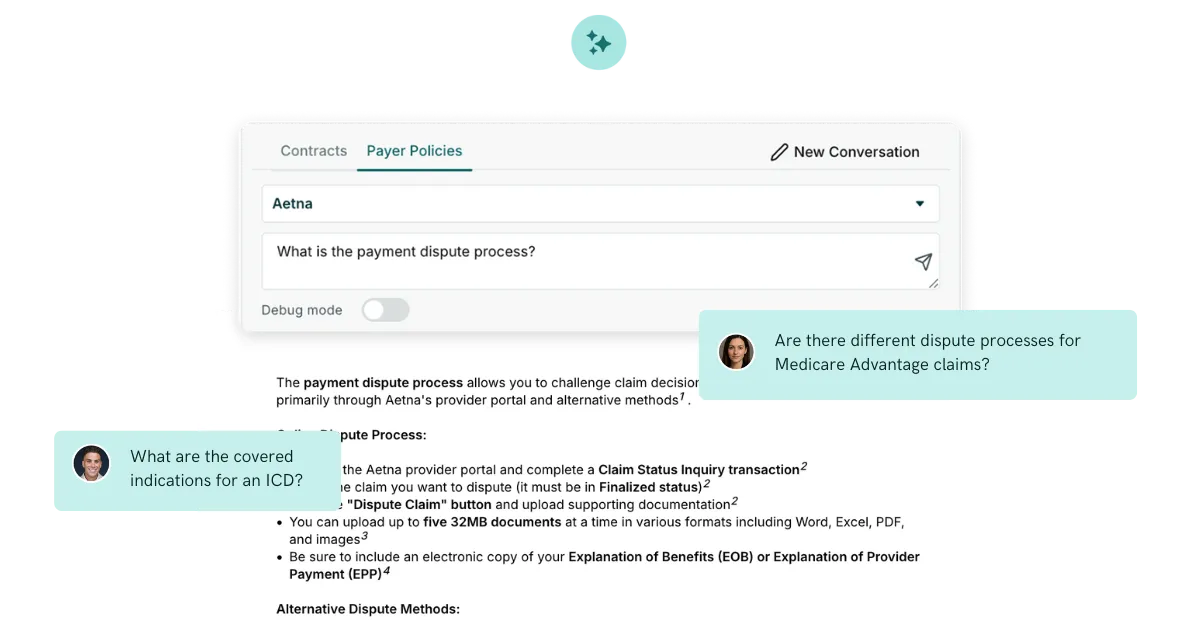
And as we’ve seen from our customers, when payers and providers share data through transparent schemas, workflows speed up. When contracts are structured, negotiation stops being guesswork and starts being strategy. When AI is applied to that foundation, it doesn’t just automate tasks, it brings consultant-grade opportunities to your computer screen faster than you can finish reading this sentence.
The right tech doesn’t make healthcare simpler by magic. It makes it simpler because it forces us to organize the complexity we’ve tolerated, and spent millions “optimizing” for decades.
That’s the frontier. Policy built the scaffolding, but the industry will build the structure and hang those family vacation photos. Reform will come not just from new regulations, but from thousands of daily choices made by analysts, negotiators, engineers, and product thinkers rewriting the system from the inside out.
At Turquoise, that’s the kind of reform we’re building for: one of contracts, workflows, and better-enabled people of healthcare, everywhere.
Interested in learning more about how we use AI to enable a more efficient healthcare backoffice? Take this self-guided demo of Clear Contracts or send us a note.
See inside the black box
Traceable data, unified workflows, and total transparency
Related resources
Learn, listen, and watch the latest on price transparency.

Introducing the Turquoise Out-of-Network Dashboard
Turquoise launched a free, open license out-of-network pricer built on data designed to eliminate the opacity in QPA calculations, IDR disputes, and broader OON pricing scenarios.


